Polymyalgia Rheumatica
What is polymyalgia rheumatica?
The term polymyalgia rheumatica is derived from Greek words, ‘poly’ means multiple, ‘my’ means muscle and ‘algia’ is related with ache and pain. Rheumatica term is related with muscle and soft tissues. Polymyalgia rheumatic is characterised by stiffening of neck, upper arm, lower back and thighs. It induces muscle pain. Rapid progression of symptomatic approaches occurs and condition worsens in the morning. It is hard to diagnose as it is not associated with joint inflammation.
Elderly persons with more than 65 years of age mainly complain about polymyalgia rheumatic, but rarely developed in early age or even not before 50 years of age. Often case reports revealed that polymyalgia rheumatic is linked with giant cell arteritis, almost 20% of case reports supports the fact.
Symptoms
Symptoms development of polymyalgia rheumatica is quick and a sudden onset of disease converts a healthy person to polymyalgia rheumatic patient by one morning attack. The patient with Polymyalgia rheumatica often complains the following symptoms:
- Stiffness in the shoulder and neck
- Pain or ache in neck, shoulder, and upper arm which extends up to lower body parts including lower back, hips and thighs
- Restricted movement of the affected parts
- Less commonly affects wrist, elbow and knee
- Disturbed sleep
The progression of the disease associated with following symptoms
- Weakness
- Anorexia
- Weight loss
- Lethargy
- Mild fever
- General malaise
- In prolong condition depression may occur.
Polymyalgia rheumatica is often associated with giant cell arteritis and onset of both the diseases increase the symptomatic approaches which include headache, tenderness in scalp, jaw pain and vision disturbances.
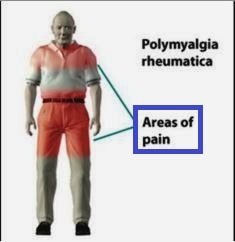
Image 1: Pain in polymyalgia rheumatica
Causes
The exact reason of development of the polymyalgia rheumatica is yet to discover. Some findings suggested that HLA-DR4 haplotype, elevated level of IL-6 are associated with polymyalgia rheumatica. These aggravate the symptoms of polymyalgia rheumatic. Non-erosive synovitis and tenosynovitis are accountable to develop many symptoms of polymyalgia rheumatic.
The possible considerable causes are:
- Genetic factors. It has been suspected that certain genetic arrangement or variations often increase the probability of development of the polymyalgia rheumatic.
- Environmental factors. It has been observed that development of the symptoms of polymyalgia rheumatica is related with seasonal changes. Environmental virus attack can cause polymyalgia rheumatica though the specific virus identification is yet not possible.
- Current study recommended that the initial beginning of pain at the shoulder and hip joints extends up to neck, upper hand and thigh due to development of the referred pain.
Diagnosis
- Diagnosis is very difficult as symptoms are linked with other diseases. During physical examination, doctors mainly check the immobility or degree of stiffness at the particular region. The proximal hip/leg and/or shoulder/arm girdle often become tender which can be felt by touching the area.
- The usually recommended diagnostic approaches are related with blood tests and specifically conducted for:
- Erythrocytes Sedimentation Rate and report is high than the normal in such cases.
- Estimation of C-reactive protein, or CRP and elevated report shows the internal inflammatory factors increment.
- Complete blood counts
Other than these blood tests, X ray, ultrasound and MRI is conducted for more accurate diagnosis. If the polymyalgia rheumatica is related with Giant cell arteritis, then biopsy of the affected artery is conducted and eye sight checking is very important to control the complication.
Treatment
Treatment helps to control the symptoms but usually such conditions gets reversed.
The usual recommended medication is steroidal drugs to control the pain and stiffness. The route of drug administration is oral and prednisone and other corticosteroids are the most preferable drug for the choice of treatment. Daily dose depends upon the patient’s condition which may extend for minimum 10 mg to 20 mg per day. The initial response is commonly quick within 2 to 3 days. Initially the dose is higher and gradually get decreased as the dose of steroidal drugs has more side effects. Doctors often prescribed the drugs in such a manner that relapsing of the symptoms should be low with minimum effective dose.

Image 2: Steroid injection in treating polymyalgia rheumatica
The included side effects of steroidal drugs are increased body weight, bones becoming fragile and development of the osteoporosis, elevated blood pressure, and blood sugar level increase and there is chances of the development of the cataracts in the eye. To control the bone health, doctors often recommend calcium and vitamin D supplements.
Other drugs which may be prescribed along with corticosteroids are methotrexate, which is an immune-suppressing medication that helps to prevent the degenerative condition associated with steroidal drugs. Anti-TNF drugs are also prescribed for those who cannot tolerate steroidal drugs including diabetic and osteoporosis patients.
Non-steroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen and naproxen (Naprosyn, Aleve) are mostlt unable to control the symptoms arises in case of polymyalgia rheumatica.
Physiotherapy
Physiotherapy helps to reduce the pain and also restore the muscle strength, coordination and improving the capability to carry out daily activities.
Diet
Restricted diet also improves the condition and chances of relapsing. It is advisable to take low salt diet to prevent fluid retention and hypertension. Fat rich diet is not recommended to the patient with Polymyalgia rheumatica. The following items should be included in diet such as:
- Fresh fruit
- Green vegetables
- Cereals
- Low fat meat
- Dairy products
Prognosis
Elderly patients are mostly affected with polymyalgia rheumatica, mostly patient above 65 years of age reports this disorder. The incidence rate is double in women than men. White race people are more commonly affected with this disease.
References
- http://www.arthritis.ca/page.aspx?pid=958
- http://www.rheumatology.org/I-Am-A/Patient-Caregiver/Diseases-Conditions/Polymyalgia-Rheumatica
- http://www.mayoclinic.org/diseases-conditions/polymyalgia-rheumatica/basics/treatment/con-20023162
- http://emedicine.medscape.com/article/330815-clinical#b4
- http://www.nhs.uk/conditions/Polymyalgia-rheumatica/Pages/Introduction.aspx
