Giant Cell Arteritis
What is giant cell arteritis?
Giant cell arteritis represents the cranial artery which passes through temporal lobe become inflamed. Artery is responsible for carrying oxygenated blood from heart to different tissues.
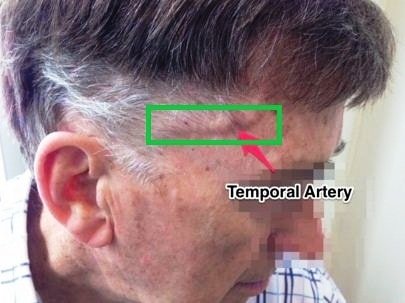
In giant cell arteritis part of brain affected due to lack of oxygen and prolong untreated condition causes tissue necrosis which leads to various complications. Brain is controlling our other organs activity and most of the cases giant cell arteritis provides vision disturbances, jaw pain, headache and even stroke can also occur. The onset of disease is most frequent in elderly persons.
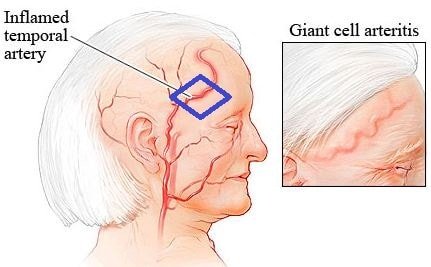
Image 2: Giant cell Arteritis
Symptoms
The symptoms are varied from individual to individual. At the initial stage, individual feels general malaise with flu like symptoms which include headache mainly started from both sides of the head and extends up to frontal region. Initial diagnosis and treatment can restrict the complications which are associated with advanced stage of giant cell arteritis.
General symptoms of giant cell arteritis are
- Head ache
- Tenderness at the both temporal lobes of the skull
- A cord like structure hurting during sleeping, keeping head against pillow or combing of hairs.
- Chewing difficulty due jaw pain
- Vision disturbance
- Muscle stiffness
- Body ache
- Fever
- Weight loss
It has been reported that most of the giant cell arteritis is combined with polymyalgia rheumatic. Association of both diseases, causes a wide range of symptoms. Stiffness and ache in the neck, shoulder, and upper arm which extends up to lower body parts including lower back, hips and thighs are included with above mentioned symptoms in combination of both the diseases.
Giant Cell Arteritis Causes
The exact cause of giant cell arteritis is not known, but it has been hypotheses that infection and autoimmune disorder associated with giant cell arteritis.
Giant cell arteritis is mainly an ailment occurs due to cell-mediated immunity. It is hypothesized that endothelial injury causes a maladaptive response and leads to actinic damage in the temporal artery. It is estimated that one of the reasons of this damage is chronic sun exposure. The initial immunological disorder occurs at the adventitia and gradually extends to intima and media of the affected artery. Autoimmunity where body’ own immune system damaged the arterial structure linked with aging, as the prevalence of the disease mainly occurs after age of 50 years.
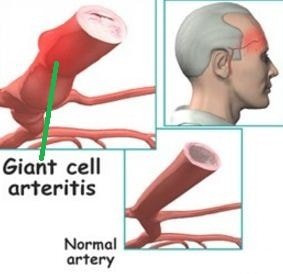
Decrease blood flow increases the stain in the wall of the artery and causes inflammation. In giant cell arteritis, temporal artery gets affected.
Diagnosis
To diagnose the giant cell arteritis, physical examination and laboratory tests both are important.
Physical Examination
Touching at the affected temporal region, finding of cord like structure and feeling of tenderness in the affected artery or arteries is prominent. The pulse rate of the affected artery is also slowed down.
Blood Tests
To check the severity of the internal inflammation, erythrocyte sedimentation rate and C reactive protein estimation is conducted. Usually both the test results have higher value than the normal in giant cell arteritis.
Decrease the number of red blood cells also causes inflammation in the artery.
Biopsy
Biopsy is conducted to get the knowledge about abnormal cell growth in the affected artery of the temporal lobe. In this process tiny section of the affected artery is examined under the microscope. For confirmation may be more than one biopsy conducted.
Above mentioned three tests are mostly conducted in giant cell arteritis, other than these, doctors may suggest conducting the following tests:
- Magnetic resonance angiography (MRA). This test is a combination of MRI and contrast material which provides comprehensive images of the artery.
- Doppler ultrasound. This test is conducted by utilizing sound waves which generates images of blood circulation via blood vessels or artery.
- Positron emission tomography (PET). Intravenous administration of radioactive material in very small quantity which helps to identify the inflamed area by providing detailed images through PET scan.
Treatment
Vast verities of medications are not available in the treatment of giant cell arteritis. To treat the condition limited medication options are present with a wide range of side effects, doctors must care about the treatment procedure and follow up to monitor the recurrence of the symptoms and control the side effects.
Steroidal Drugs
Initially to control the symptoms, steroidal drugs which include prednisone, corticosteroids are given in high doses, almost 40-60 milligram per day. When the condition becomes controlled, then a gradual reduction of dose is very important to lessen the side effects. Some prominent side effects, include weight gain, fragile bone structure, decrease calcium level, etc. To control the side effects, doctors often prescribed calcium and vitamin D supplements along with steroidal drugs.
Steroidal complications also include weight gain, hyperglycaemia, hypertension and fluid retention, which can be controlled by restricted food habits which include limit in sugar, salt and fat containing diet.
Immunosuppressant agents
To restrict the steroidal complications or those who required long term, high dose of steroidal treatment, for them immunosuppressant agents are used. Cyclosporin, azathioprine, methotrexate are the example of immunosuppressant agents which can be prescribed in advance stage of giant cell arteritis.
Prognosis
The exact cause of development of the giant cell arteritis is unknown, but it has been predicted that genetic, environmental, and autoimmune factors triggering the disease process by enhancing the inflammatory cascade.
The incidence rate is high in Europe and United States compare with African Americans. The affected patient is mostly older adults; the incidence rate is high in the age between 65 to 75 due to swelling and stiffening of the temporal artery. Rarely individual under 50 years of age gets affected with giant cell arteritis.
References
- http://emedicine.medscape.com/article/332483-overview#a3
- http://www.arthritis.org/about-arthritis/types/giant-cell-arteritis/
- http://patient.info/health/giant-cell-arteritis-leaflet
- http://www.mayoclinic.org/diseases-conditions/giant-cell-arteritis/basics/causes/con-20023109
- http://www.nlm.nih.gov/medlineplus/giantcellarteritis.html
