Myotonic Muscular Dystrophy
What is myotonic muscular dystrophy?
Muscular dystrophy is associated with progressive muscle degeneration followed by muscle weakness. One of the most common types of muscular dystrophy that affects in adult is myotonic muscular dystrophy (MMD), but there is a chance of congenital abnormality also.
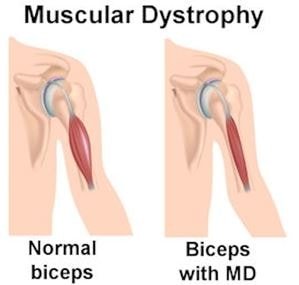
Usually the symptoms are mild and not dangerous like other muscular dystrophy. The alternative name of this disorder is Steinert’s disease. In myotonic muscular dystrophy, patient unable to have relaxed muscle and contracted form of muscle hampers the normal functioning of the muscle. The first onset of the symptoms is mainly restricted in facial and neck muscle followed by other part of the body.
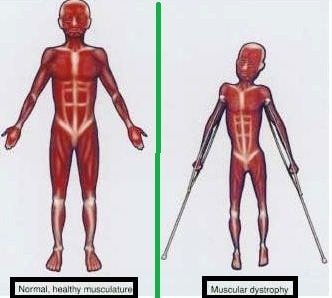
Image 1: Muscular dystrophy
Causes
When the two responsible genes are not in their proper size and one of the genes is larger than its normal size then it results to the myotonic muscular dystrophy.
In case of congenital (MMD), one of the common finding is that mother suffers with adult-onset MMD. Sometime due to mild symptoms, patient is unaware of the disorder. If the adult-onset MMD is present in mother or father, both can transfer the disorder to child. Mother is responsible for congenital onset or adult onset MMD and in rare cases; father is responsible for adult –MMD.
Type 1, Type 2
Myotonic muscular dystrophy is of two types – Type 1 and Type 2. Both the types are caused by genetic autosomal abnormality, which means that the responsible gene mutation abnormality in due to one copy that can be able to cause the disorder. Usually one of parents is having the disorder.
Type 1
this type is generated due to one gene from chromosome 19, termed as DMPK becomes abnormally elongated. The exact function of DMPK is not known, but is has been found that protein synthesized by this gene is responsible to communicate the cell functioning. This is important for heart, skeletal muscle and brain muscle contraction and relaxation.
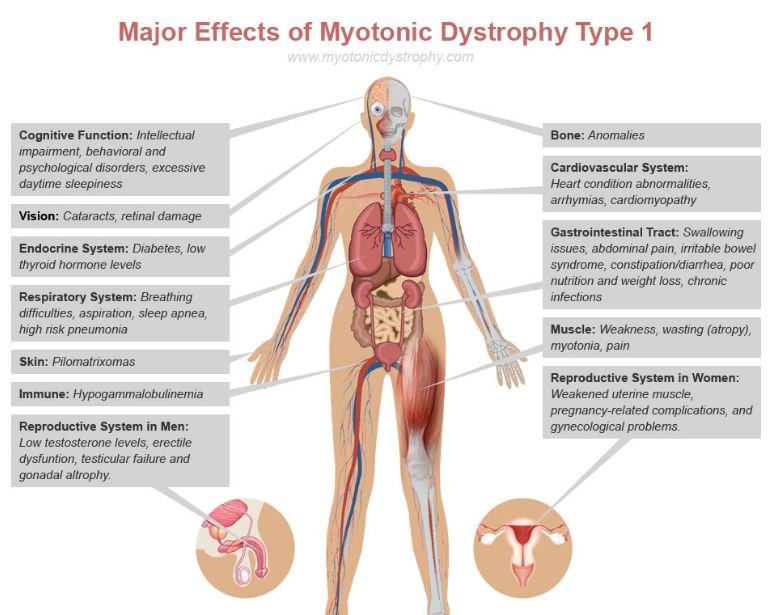
Type 2
In this type, genes present on chromosome 3 termed as CNBP or ZNF9 that become elongated in size. Type 2 is also termed as proximal myotonic myopathy (PROMM). In heart and brain, mainly the CNBP gene synthesizes a protein which helps to regulate the functioning of the other genes.
Type 2 is milder than type 1 and even sometimes presence of type 2 not even produce any symptoms.
Symptoms
Myotonic muscular dystrophy produces very low disability than any other muscular dystrophy. The disease progression is also very slow.
Limb disability
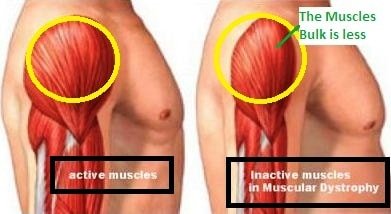
Image 4: Affected muscles in the muscular dystrophy
- Arm and leg both the limb muscles become weak.
- The forearm, lower leg, hand and sole muscles are thinner and weak due to shrinkage of the muscle than the other adjoin part of the limb; as these parts are distend from the center part of body.
- The grip of the hand is weak.
- The walking speed is slower
- Poor handwriting due to holding problem of pen or pencil.
Facial muscles
- Long thin facial appearance
- Ptosis or Eyelids droops which causes difficulty to open eye during watching TV or reading of a book.
- Temples of skull become concave.
- Holding of head become tough due to weakness in the neck muscles.
Respiratory muscles weakness
- Feel sleepy due to less of oxygen intake.
- sleep apnea (cessation of breathing for few seconds to minute during sleep)
Oesophagus Weakness
- Swallowing difficulty
- Chocking
- Vomiting is fatal for them
Heart problem
- The electric impulse generation and transmission related problems are more prominent in advanced stage of type 1 MMD. For this reason, abnormality in heartbeat is common in adult aged MMD patients.
Learning disability
- Not prominent in adult aged MMD
- Congenital abnormality and onset of disease in early childhood causes learning disability in suffered children
Treatment
There is no specific treatment for MMD, symptomatic treatment is usually given to a patient to lessen their disability and for restricting the associated complications.
- Walkers, braces, Canes and scooter are the different accessories which may reduce the patient’s mobility problem.
- Medications are given to treat constipation and other gastro-intestinal diseases.
- Cataract surgery is needed for those who develop cataract development.
- Medications are available to treat excess sleepiness.
- Periodic monitoring of respiratory function is very important to control the respiratory cessation.
- Cardiac problem can be controlled by routine cardiac function monitoring.
Prognosis & Life Expectancy
The incidence rate is more in Type 1 than the type 2, it has been estimated that 1 in 8000 people suffer from MMD. The type 2 is more common in Finland and Germany.
The life expectancy depends upon the severity of the disease syndrome. Usually people are having normal life expectancy in case of mild syndrome.
References
- http://www.mayoclinic.org/diseases-conditions/muscular-dystrophy/basics/symptoms/con-20021240
- https://www.mda.org/disease/myotonic-muscular-dystrophy
- http://ghr.nlm.nih.gov/condition/myotonic-dystrophy
- http://mdaustralia.org.au/wp-content/uploads/2012/07/013_myotonic-dystrophy-2012.pdf
