Keratoacanthoma
What is Keratoacanthoma?
Keratoacanthoma abbreviated as KA and also called as molluscum sebaceum, refers to a tumor on the skin considered as low-grade type since it does not metastasize to other areas and which originated from the hair follicle neck portion or the pilosebaceous glands of the skin. KAs grow fast and they are called squamo-proliferative type of skin lesions which are taking a similar form of the pathological presentation of squamous cell carcinomas.
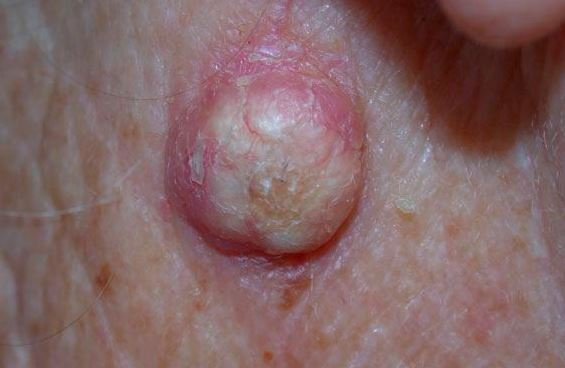
KA is being characterized to take its rapid growth within the range of just a few weeks, taking an approximate measure of 1cm to 2cm going into a few months, where most cases can have a range over 4 months to 6 months of spontaneous resolution. KAs are harmless epidermal growths that a person does not have to worry much, as this lesion rarely spreads itself and is quickly removed by physicians upon early detection.
Histology
Keratoacanthomas which are clinically diagnosed under a microscope study are found to be a well-differentiated type of squamous cell carcinoma. It consists of a crater that is filled with keratin and with keratinocytes which are well-differentiated, extended on all sides of the crater-lip with no evidence of dermal invasion on other areas.
Pathologists have classified KA as a distinct type of skin lesion and are not malignant and labeled it specifically as a well-differentiated squamous cell carcinoma with a keratoacanthoma variant.
Based on some studies, about 6% of the cases of KAs both with clinical and histological background have progressed to the invasive type of squamous cell cancer. Thus, prompt management through surgical removal of the KA is highly recommended.
Causes
There are instances where the cause of KA is not known as it develops. KAs can happen to a person due sun exposure and to those who are working or exposed with carcinogenic chemicals. Others can have KA because of trauma experience, some genetic traits in the family and those diagnosed with the human papillomavirus or any immunocompromised health status can also have the KA in them.
The incidence presents an estimate ratio between 1:1000 among the cases. KAs are usually noted among older adults over 60 years and very rare in young adults. It is not common to patients who are darker-skinned. The chances of the males to have KA are twice more than the females. Some new treatments available for melanoma have been associated to predispose a person to have KA, especially those prescribed with Dabrafenib and Vemurafenib drugs.
Signs and Symptoms
Keratoacanthomas can be grouped according to the different types depending on its manifestation:
- Giant KA is a variant KA with several centimeter dimensions
- Keratoacanthoma centrifugum marginatum is a cutaneous KA with multiple tumors localized in one area
- Multiple keratoacanthomas is a cutaneous KA with multiple to hundred KAs growing in one area
- Solitary keratoacanthoma is a non-malignant rapid growing tumor usually located in the nails
- Generalized eruptive keratoacanthoma is a cutaneous KA with hundreds to thousands of keratotic papules distributed all over the body
How is Keratoacanthoma being diagnosed?
Attending physicians usually prefer and perform a skin lesion biopsy, instead of the KA shave biopsy. The rationale is for analysis of the lesion to confirm a diagnosis of KA. The differential diagnosis done is to specify the squamous cell carninoma from the other types of skin lesions.
Treatment
Surgical removal of the skin lesion is the main modality of approach for KA. Physicians will have to perform a complete excision for all skin lesions which are confirmed to be growing keratoacanthomas. The removal of the full lesion, following adequate margin, removes the lesion, giving time for tissue diagnosis and a surgical wound can be repaired with cosmetic results advantageous for the patient.
The use of medical treatment through medications is being reserved in cases where surgery is not a possibility because of the location or distribution of the skin lesions or tumor. Systemic retinoid drugs can be prescribed for patients with numerous lesions in the body. In cases where surgery is not possible to be performed, the following medicines are directed to use:
- Intralesional methotrexate 5-fluorouracil
- Steroids
- Bleomycin
Alternative therapies available for KAs:
- Electrodesiccation and curettage
- Cryotherapy
- Laser therapy
- Radiation therapy
Pictures
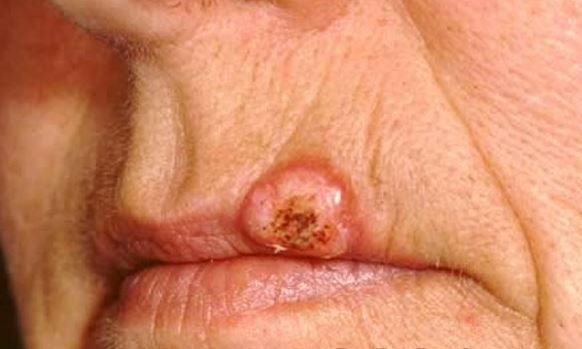
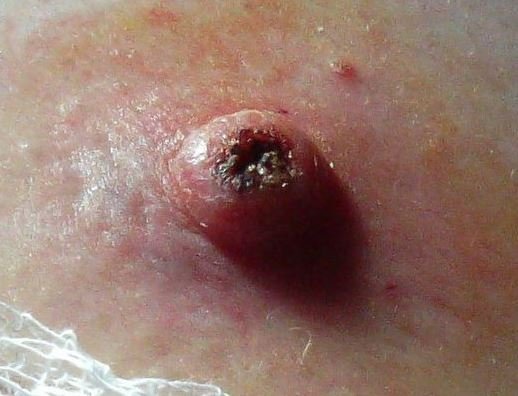
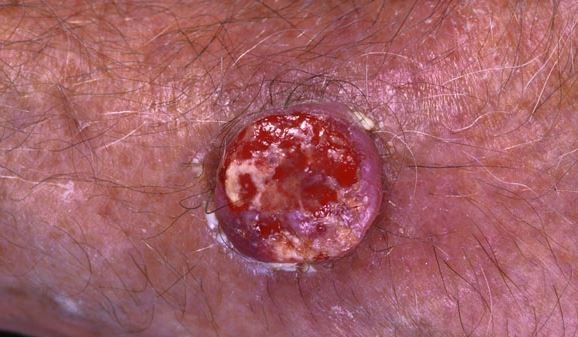
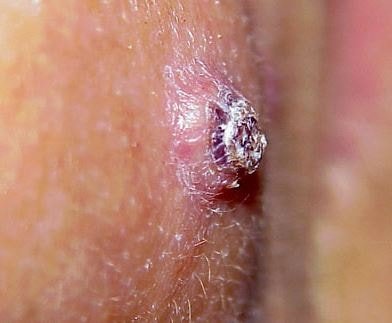
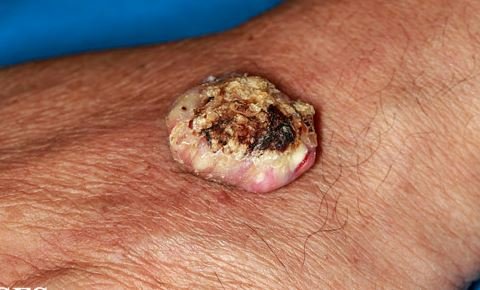
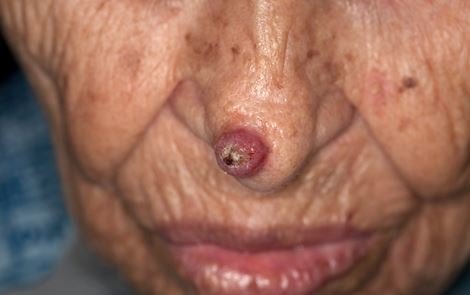
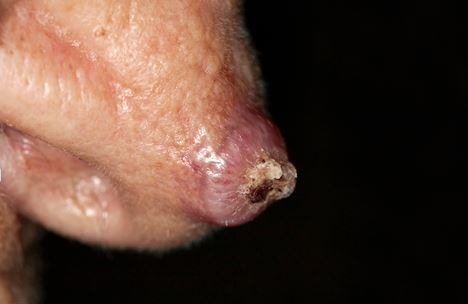
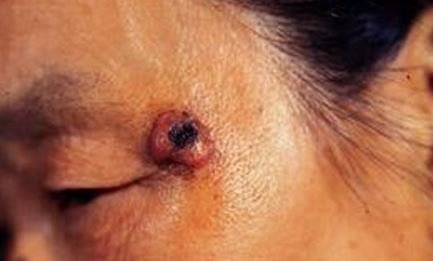
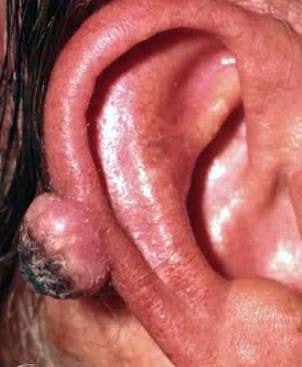
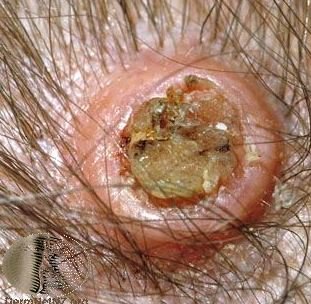
References
- http://emedicine.medscape.com/article/1100471-overview
- http://patient.info/doctor/keratoacanthoma-pro
- http://www.healthline.com/health/keratoacanthoma#Overview1
- Weedon DD, et al (2010). Squamous cell carcinoma arising in keratoacanthoma: a neglected phenomenon in the elderly. Am J Dermatopathol. 32(5):423–6.
- Kossard S; Tan KB; Choy C (2008). Keratoacanthoma and infundibulocystic squamous cell carcinoma. Am J Dermatopathol. 30(2):127–34 (ISSN: 1533-0311)
- James, William; Berger, Timothy; Elston, Dirk (2005). Andrews’ Diseases of the Skin: Clinical Dermatology. (10th ed.). Saunders. ISBN 0-7216-2921-0.
