Strawberry Cervix
Introduction
Strawberry cervix is one of the changes that may happen to the cervix due to a presence of an infection. If this change is noticed in the cervix, it is important to consult a physician in order to receive the appropriate treatment for the infection [1].
What is Strawberry Cervix?
Strawberry cervix, or colpitis macularis, is the appearance of punctate hemorrhages in the cervix and vagina. These petechial lesions give the strawberry-like appearance to the cervix. This condition is very different from the general inflammation of the cervix because this condition is associated only with Trichomonasis infection. Around 25% of women who have this infection, present with a strawberry cervix. Figure 1 shows the typical appearance of a strawberry cervix [1, 2].
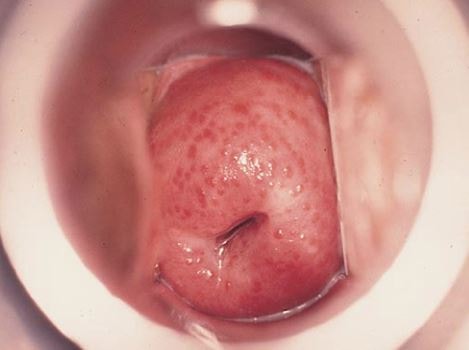
Causes of Strawberry Cervix
The pathogen that is responsible for the strawberry cervix is the Trichomonas vaginalis. This organism is a one-cell parasite that affects both females and males. In females, the usual areas that is affected by this organism are the vagina, cervix, urethra, bladder and glands in the genital area. For the males, the urethra and the area under the foreskin of those who are uncircumcised are the most affected [3, 4].
The pathogen is passed from one person to another primarily through sexual contact. The use of protective devices such as condoms will help prevent acquiring the disease. Although it rarely occurs, it can be acquired by using the personal items of an infected individual such as a wet towel. This protozoan is able to survive out of the human body for 45 minutes which makes the transmission through personal items possible. Another method of transmission is through the vaginal birth of an infected mother. [3]
Signs and Symptoms of Strawberry Cervix
There will be microscopic, punctate hemorrhages on the cervix and it will give a strawberry-like appearance to the cervix [3, 4]. Other symptoms that may be experienced with a strawberry cervix are:
- Malodorous vaginal discharge
- Itching in the vaginal area
- Painful or difficult urination
Diagnosis of Strawberry Cervix
Health History and Physical Examination
The focus of the health history is the sexual history because a most Trichomoniasis infections are transferred sexually. Physical examination involves inserting a speculum in the vagina to observe for any changes. The vagina and cervix will be distinct and inflamed and will have red blotches on the wall. A sample of the vaginal discharge will be obtained and be subjected for further tests [5].
pH Test
The pH level of the vaginal discharge can help determine the presence of an infection. Normal vaginal discharge should be 4.5 or less. If the pH level is higher than this, it may indicate that there is an infection that is present [5].
Whiff Test
After using the vaginal speculum in the physical examination, there will be some discharge that will accumulate in the lower lip of the speculum. The odor of this sample will be taken and it will be considered as a positive whiff test if it possess a pungent, “fishy” odor [5].
Wet Mount
The wet mount method is the diagnostic test that is most preferred by physicians because it has a sensitivity ranging from 50- 90%. A small amount of the vaginal discharge will be used to make a wet mount. This will be placed under a light microscope and it will be able to show the presence of the pathogens. The rapidly moving organisms in the mount are the Trichomonas vaginalis [5].
Treatment of Strawberry Cervix
The primary medication that will be prescribed to resolve the infection are metronidazole or tinidazole. These are usually in the form of pills, tablets or capsules and taken orally. Alcohol should not be taken for 24 hours after taking metronidazole or 72 hours after taking tinidazole because it can lead to nausea and vomiting. Medications that are inserted through the vagina are meant to relieve the symptoms and not resolve the infection. It is essential to complete the whole course of the drug treatment to treat the infection [3, 6].
Prevention of Strawberry Cervix
The risk for re-infection for trichomoniasis is around 36%. This can be prevented by avoiding sexual contact with an infected individual. The use of protective methods such as a condom will prevent from acquiring the infection but the best way is to abstaining from sex [3, 6].
References
- Casey, P., Long, M., & Marnach, M. (2011). Abnormal Cervical Appearance: What to Do, When to Worry? Mayo Clinic Proceedings, 147-151.
- Neinstein, L. (2013). Sexuality – Sexually Transmitted Infections – Vaginitis (B3). Retrieved from Adoslescent Health Curriculum: https://www.usc.edu/student-affairs/Health_Center/adolhealth/content/b3stis3.html
- Healthwise Staff. (2012, July 9). Trichomoniasis . Retrieved from emedicinehealth: http://www.emedicinehealth.com/trichomoniasis-health/page11_em.htm
- Swygard, H., Sena, A. C., Hobbs, M. M., & S, C. M. (2004). Trichomoniasis: clinical manifestations, diagnosis and management. Sexually Transmitted Infections, 91-95.
- (2015). Diagnostic Tests. Retrieved from Stanford: http://web.stanford.edu/group/parasites/ParaSites2002/trichomoniasis/Diagnostic_Test.html
- Cirino, E. (2016, February 22). Trichomoniasis in Pregnancy. Retrieved from Healthline: http://www.healthline.com/health/pregnancy/infections-trichomoniasis#Overview1
