Ecthyma Gangrenosum
Ecthyma gangrenosum is a manifestation of the systemic sepsis caused by the pathogen Pseudomonas aeruginosa. This condition most commonly affects individual who have a compromised immune system and rarely affects healthy individuals [1, 2, 3].
Anatomy and Pathophysiology
Ecthyma gangrenosum is the appearance of bloody pustules that may develop into black necrotic ulcers. This condition is associated to a systemic infection of Pseudomonas aeruginosa and the ones who are usually affected are those who are either immunocompromised or critically ill. The impaired cellular or humoral immunity of individuals with compromised immune system makes them susceptible for this condition.
Bacterial invasion of the blood vessels causes the necrotizing vasculitis. Aside from this, the breakdown of the body’s defense mechanism such as the skin may even allow the spread of the pathogenic organism. Edema and the necrosis may also cause an interruption of the blood supply to the affected tissues. This event may result to necrosis of the dermis and epidermis which can be seen as nodular lesions that undergoes the process of hemorrhage, ulceration and tissue death [2, 3].
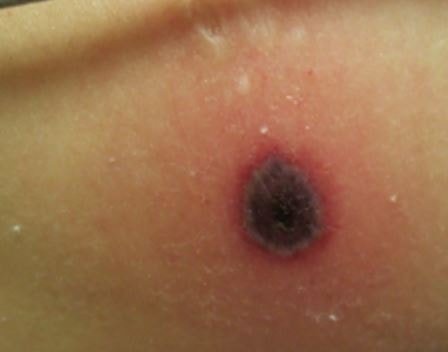
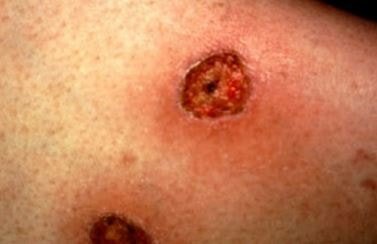
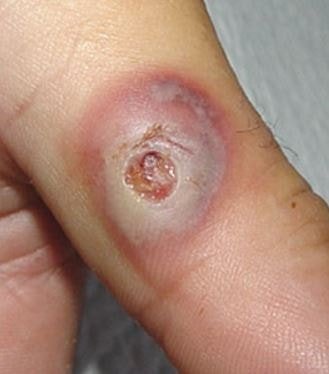
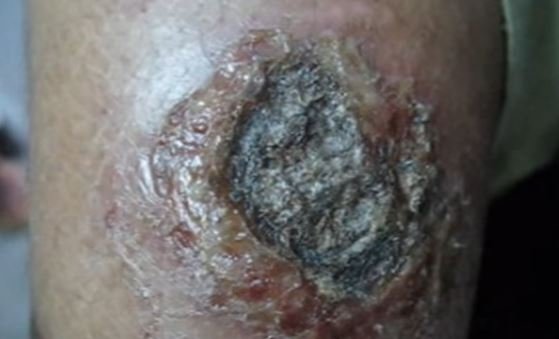
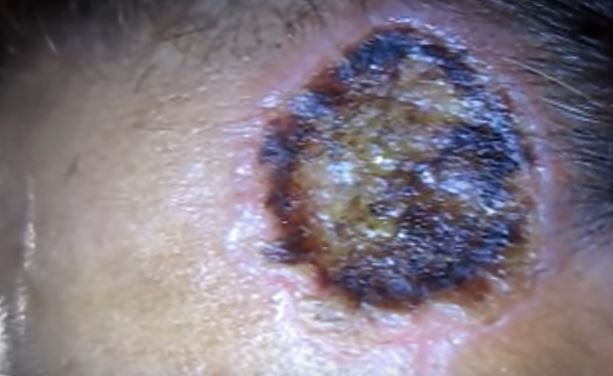
Figure 1 shows the lesions of ecthyma gangrenosum.
This condition can be seen from around 13% of people who have a pseudomonas systemic infection. There are reports of ecthyma gangrenosum in otherwise healthy children but most of them either have a recent viral disease or is undergoing an antimicrobial therapy for other conditions. It may be present in all ages but they are more common in elderly patients and infants because of their compromised or immature immune system [2, 3].
ICD10 Code
The diagnosis code that is used for this skin condition is L08.0. This code is used for any purulent conditions of the skin [4].
Causes of Ecthyma Gangrenosum
Pseudomonas aeruginosa may be the primary cause of ecthyma gangrenosum but this condition is also seen in systemic infections caused by other pathogens [3, 5].
- Gram-positive bacteria: Streptococcus pyogenes, Staphylococcus aureus
- Gram-negative bacteria: Chromobacterium violaceum, Escherichia coli, Aeromonas hydrophila
- Fungi: Mucor and Rhizopus sp, Aspergillus fumigatus, Candida albicans
- Virus: Herpes simplex
Signs and Symptoms
The primary lesions of ecthyma gangrenosum may appear initially as red, round, painless patches which may become pustular surrounded with redness. A hemorrhagic focus will form into the center which will eventually develop into a blister. The blister will spread peripherally and will evolve into a gangrenous ulcer. Other characteristic of this ulcer is a black or gray scab that is surrounded with a red halo. The transition is fairly quick in such that a lesion will turn into a necrotic ulcer in as fast as 12 hours [3, 5].
Lesions may appear at any site in the body but they are most commonly found under the armpits and in the anogenital area. The extremities, face and trunk are usually less involved with ecthyma gangrenosum. Development of lesions in the periorbital area may be rare but its occurrence have been reported [3, 5].
Diagnosis of Ecthyma Gangrenosum
Health history and physical examination
Patients who present with lesions associated with ecthyma gangrenosum are investigated for the presence of systemic infections. Factors which may lead to the breakdown of the skin will be identified as well. The whole body will examined to assess the lesions in the body [3, 5].
Gram stain
A sample of the fluid found on the central hemorrhagic blister or pustule will be sent to the laboratory. If there is no pustule, a scab may be used instead. This test will be able to identify the pathogenic organism [5].
Skin Biopsy
A biopsy may be performed on a skin sample. It will undergo a routine histology and stains to rule out the possibility of a bacteria or fungi which may cause lesions with the same characteristics. A histopathology performed on ecthyma gangrenosum skin sample will show necrosis of the blood vessels with some inflammatory cells present. There will be a good number or surrounding bacteria that are present [5].
Blood and Tissue Cultures
The specimens should be obtained prior to starting any antibiotic therapy. This tests will be able to identify the strain of bacteria or fungi that is the cause of the infection. A sensitivity test will be performed on the pathogen that was identified [5].
Treatment of Ecthyma Gangrenosum
This skin condition requires immediate diagnosis and treatment. The result of the culture and sensitivity test will be able to tell the most appropriate antibiotic agent to be used. The presence of ecthyma gangrenosum on an individual should alert the physician to check for the presence of a systemic infection. Examples of the drug that may be given are antipseudomonal penicillins, fluoroquinolones, aminoglycosides, aztreonam or a third-generation cephalosporins.
If a culture and sensitivity test is not performed, the patient may undergo an empiric antifungal and antimicrobial therapy. In doing so, the drug that should be used should be able to cover all the likely pathogens taking the clinical setting into consideration. If the lesions failed to respond to the drug therapy, a surgical debridement of the necrotic lesions may be performed by the physician [3, 5].
Ecthyma Gangrenosum Pictures
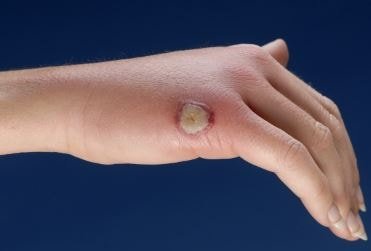
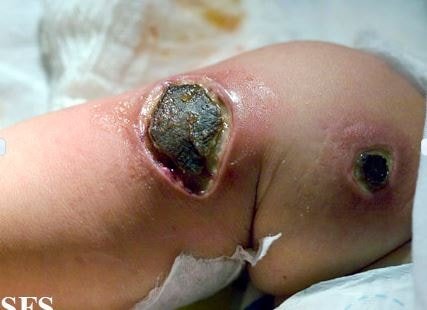
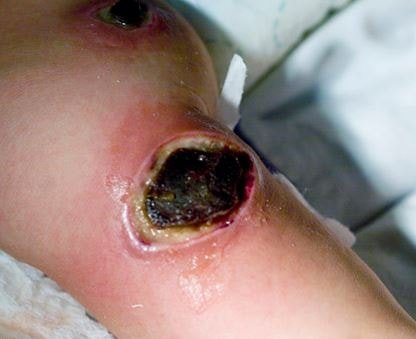
References
- Varghese, G., Eapen, P., & Abraham, S. (2011). Ecthyma gangrenosum of a single limb. Indian Journal of Critical Care Medicine, 188-189.
- Chan, Y., Chong, C., Puthucheary, J., & Loh, T. (2006). Ecthyma gangrenosum: a manifestation of Pseudomonas sepsis in three paediatric patients. Singapore Medical Journal, 1080-1083.
- Kingsbery, M. Y. (2015, November 18). Ecthyma Gangrenosum. Retrieved from Medscape: http://emedicine.medscape.com/article/1053997-overview#a4
- ICD10 Data. (2015). Pyoderma. Retrieved from ICD10 Data: http://www.icd10data.com/ICD10CM/Codes/L00-L99/L00-L08/L08-/L08.0
- Duffill, M. (2015, November 29). Ecthyma gangrenosum. Retrieved from Derm Net NZ: http://www.dermnetnz.org/bacterial/ecthyma-gangrenosum.html
