Hyaline Casts
A urine analysis is a screening tool that analyzes the components of the urine. The results of this test may reveal the presence of certain particles that indicate an underlying condition that an individual may unknowingly suffer [1].
What is Hyaline Casts in the urine?
Casts are cylindrical—shapes structures that are mainly made up of the Tamm-Horsfall mucoprotein and are secreted mainly by epithelial cells. The casts are primarily produced in different parts of the kidney. These parts include the collecting ducts, distal tubules and loops of Henle. There are several types of casts and they differ in size depending on the area of the kidney where they are formed [2].
Hyaline casts are produced if the cells of the tubular lumen are absent. Upon closer look, hyaline casts have a smooth texture and they possess parallel sides and edges that are round. The length of hyaline casts greatly varies and they are usually straight but there are occasions where they are found to be rounded and convoluted.
Due to its refractive medium, these casts may be hard to see in wet preparations of the urine and there may be a need to reduce the lighting to be able to see the casts.
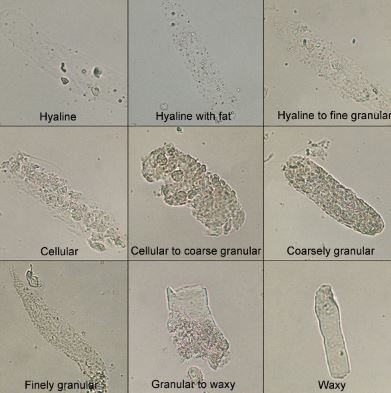
Figure 1 shows an image of a hyaline cast under a microscope [2, 3].
Hyaline Casts Urine Examination
The urine that should be used for this examination is the first morning urine. The sample should be collected through a clean-catch technique and be submitted to the laboratory within an hour of collection. There is a special kit that contains a sterile cup and wipes and it contains instructions on how to collect the sample. It is important to follow the guidelines very carefully to avoid contaminating the sample [4, 5].
This technique is done to maintain the sterility of the urine. Before getting the sample, there is a need to wash the hands. For the female individuals, the vaginal area needs to be wiped with the sterile wipes from the front to the back.
For uncircumcized men, there is a need to retract the foreskin. The tip of the penis should be cleaned using the provided wipes. A small amount of urine should be released into the toilet before consciously stopping urinating to get the midstream sample.
Care must be taken to avoid any part touching the container. Once the cup is half full, it can be placed on a stable surface while the individual finish urinating. Put the lid on the cup and label it properly. As mentioned earlier, it should be brought to the physician or laboratory as soon as it is collected [4, 5].
The urine sample will be placed in a centrifuge machine and the sediment will be seen under the microscope. Hyaline casts are counted in a low power field. The normal result is less than 5 hyaline casts for every low power field. There may be slight variations in what considered to be a normal result but the physician will be able to interpret the result of the urinalysis [4, 6, 7].
Clinical Significance
Hyaline casts of around 0-5/lpf are normally seen in the urine of healthy adults. Doing strenuous exercises may also increase the amount of hyaline casts that are excreted in the urine. These findings are not associated with any renal disease [8, 9].
If the number of these colorless and homogenous casts in a low power field is high, the patient may be suffering from a proteinuria of renal or extra-renal origin. It has been hypothesized that high levels of serum protein in the tubular lumen increases the precipitation of hyaline casts. Such event occurs in glomerular diseases and myelomas of the kidney. Dehydration is also seen to increase the number of hyaline casts found in the urine [8, 9].
A particular research done shows that the number of hyaline casts is predictive of the estimated glomerular filtration rate (eGFR) of the kidney. Individuals who have more than 100 hyaline casts/WF indicates a low filtration rate and this could suggest the progression of the kidney disease. This study has shown the importance of hyaline casts counting in diagnosing and early detection of a chronic kidney disease [10].
References
- Labtests Online. (2015). Retrieved from Labtests Online: https://labtestsonline.org/understanding/analytes/urinalysis/ui-exams/start/1#nitrite
- The Free Education Network. (2015, June 6). Urinalysis. Retrieved from The Free Education Network: http://www.free-ed.net/free-ed/Courses/06%20MedHealth/MD%20Series/MD0852/Urinalysis.asp?iNum=0302
- UOIT Clinical Biochemistry. (2015). Microscopic Urinalysis. Retrieved from UOIT Clinical Biochemistry: http://uoitclinicalbiochemistry.weebly.com/urinalysis-casts.html
- Martin, L. J. (2014, November 2). Urinary Casts. Retrieved from MedlinePlus: https://www.nlm.nih.gov/medlineplus/ency/article/003586.htm
- Kirkwood, J. (2016, January 5). Clean Catch Urine Sample and Culture. Retrieved from Healthline: http://www.healthline.com/health/urine-culture-clean-catch#Overview1
- Spencer, D. (2015). Subtopic 3: Microscopic Examination of Urine Sediment. Retrieved from Professional Development Resource by Daniel Spencer: http://www.texascollaborative.org/spencer_urinalysis/ds_sub3.htm
- Lerma, E. (2015, December 16). Urinalysis. Retrieved from Emedicine: http://emedicine.medscape.com/article/2074001-overview#a2
- The Johns Hopkins Lupus Center. (2015). Urinalysis. Retrieved from The Johns Hopkins Lupus Center: http://www.hopkinslupus.org/lupus-tests/screening-laboratory-tests/urinalysis/
- Giri, D. (2015, April 17). Type of Casts Found In Urine and Their Clinical Significance. Retrieved from LaboratoryInfo: http://laboratoryinfo.com/types-of-casts-in-urine-and-their-clinical-significance/
- Adachi, M. (2013). Clinical significance of hyaline casts in the new CKD risk classification (KDIGO 2009). Rinsho Byori, 104-111.
