Foot Fungus
Introduction
A small number of fungus is seen to be part of the normal flora of the skin, but if the skin conditions promotes the proliferation of fungus, it may overcome the defenses of the body and cause an infection [1].
What is Foot Fungus?
The overgrowth of fungus in the skin of the foot is more commonly referred to as athlete’s foot or tinea pedis. It is called athlete’s foot because it is they are the ones who often acquire this type of fungal infection. Fungi are microorganisms that eats on old and dead skin cells.
The most common types of fungi that causes athlete’s foot are Trichophyton rubrum, T. interdigitale and Epidermophyton floccosum. The presence of fungi is not enough to cause the infection, they should be able to multiply and overwhelm the body’s defense.
They thrive on a warm and moist environment such as socks, shoes, locker rooms and public swimming pool [1, 2, 3, 4].
Types of Foot Fungus
There are 3 known types of athlete’s foot [1]:
Interdigital
Considered to be the most common type, the infection occurs in the middle of the 2 smallest toes. The itching, scaling and burning in this area can spread to the sole of the feet [1].
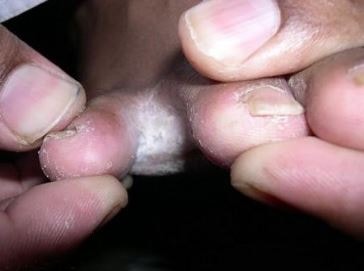
Figure 1 shows an example of an interdigital athlete’s foot.
Moccasin
Athlete’s foot of this type starts with a minor dryness, scaling, irritation and itching of the skin. As the condition progresses, it may cause thickening and cracking of the skin. Although it starts on the soles of the feet, it can extend to the sides. This type of athlete’s foot is found to be immune to some forms of therapy [1, 4].
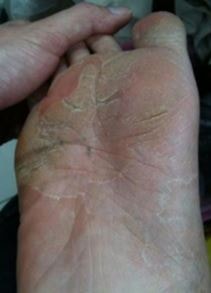
Figure 2 – shows an example of Moccasin foot fungus infection.
Vesicular
The most characteristic feature of this type is the appearance of fluid-filled blisters that usually develop on the underside of the foot. These blisters can also be found on the heel, on top of the foot and even in-between the toes [1].
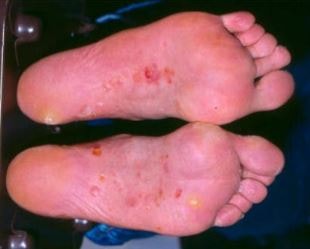
Figure 3 – illustrates an example of vesicular athlete’s foot.
ICD10 Code for Foot Fungus
The 2016 ICD-10-CM code that is being utilized for any of the 3 types of athlete’s foot is B35.3. This code may also apply to ringworm and dermatophytosis of the foot [5].
Causes of Foot Fungus
The fungi that thrives on the skin of the feet can spread to other people through direct contact with an individual who is infected or by contact through a surface that has been contaminated.
Examples of places where these fungus may be found are the warm and damp places of public pools, lockers and communal showers. Walking barefoot in these locations is one of the easiest way to acquire the microorganisms which may cause athlete’s foot [1, 2].
Getting the fungi from these places is not enough to get this infection, they would also need to thrive and multiply in these areas. Because they need moisture to survive, things that keeps the feet moist makes it a suitable environment for fungi growth.
Example of these are wearing the same pair of socks for several days, wearing tight shoes despite of feet being sweaty and not drying the feet properly after swimming in a public pool or having a shower in a communal one [1, 2].
Signs and Symptoms of Foot Fungus
Aside from the clinical features of the aforementioned types of athlete’s foot, other symptoms may include [1, 2, 4, 6]:
- Circular dry patches on top of the feet
- Peeling skin most commonly between the fourth and fifth toe
- Thick, discolored and crumbling toenails
- Toenails that may easily pull away from the nailbed
Diagnosis of Foot Fungus
Health history and physical examination
Patients consult a specialist probably due to itching and cracking of the skin on their foot. History would include knowing when the symptoms started to appear and any prior activities where the infection may have been acquired.
The physical examination will identify all the symptoms that are present in order to classify the type of athlete’s foot the patient is experiencing. A diagnosis of tinea pedis can be done through the examination of the symptoms but further tests may be done to confirm the diagnosis [1, 6].
Potassium hydroxide test
A sample of the infected skin will be scraped by the physician and will be placed in potassium hydroxide. This chemical tend to destroy the normal skin cells but leaves behind the cells of the fungi. The cells that were not damaged will be examined under a microscope to confirm if they are fungal cells [6].
Treatment of Foot Fungus
Tinea pedis can be usually treated by using over-the-counter antifungal agents. Examples of these are clotrimazole, terbinafine, miconazole and butenafine.
They are available either as a topical cream or an oral medication. If these drugs won’t resolve the infection, the physician may prescribe a stronger formulation of these medications. Other things that may be prescribed are topical steroids to reduce the inflammation in the area and an antibiotic if the open wounds and blisters have developed an infection [1, 2, 6].
Home Remedies
Aside from following the treatment regimen, the physician may recommend some of these home remedies to help alleviate the symptoms [7].
Tea tree oil
Tea tree oil contains properties that will not only help destroy the fungi that is present but will also avoid its spread to unaffected area. The foot will be soaked for 10 minutes in a foot bath that contains around 40 drops of the tea tree oil. After drying the feet, the affected area should be massaged using the oil. Doing this regularly will help hasten the healing process [7].
Apple cider vinegar and salt
These two ingredients create an environment that is too acidic for fungi to grow. This can be used either as a foot bath or a foot spray. Ensure that feet are thoroughly dried after soaking or spraying the feet. The inside of the shoes can also be wiped using this solution [7].
Corn starch or baking soda
Before wearing socks, the feet can be sprinkled with either corn starch or baking soda. It will be able to absorb the sweat and the baking soda will also able to absorb the smell of the foot [7].
Virgin coconut oil and sesame
Combining virgin coconut oil and sesame will form a solution that has antifungal properties. It is applied liberally to clean, dry feet twice a day using a cotton ball [7].
Prevention of Foot Fungus
There are measures that can be done in order to prevent acquiring athlete’s foot [1, 2, 3, 4, 6]:
- Avoid walking barefoot when going to the locker area and communal showers.
- Dry the feet thoroughly after taking a bath.
- Wear socks that are made from absorbable material such as cotton and change it every day.
- Do not wear shoes that are very tight footwear.
- Clean shoes regularly and let it dry under the sun.
Pictures of Foot Fungus
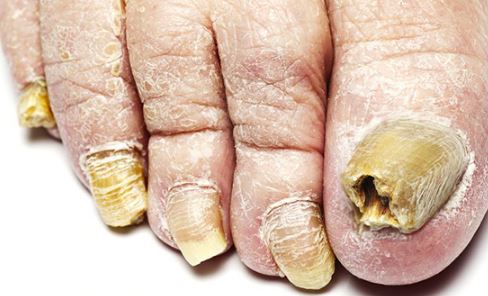
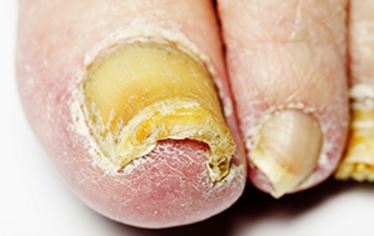
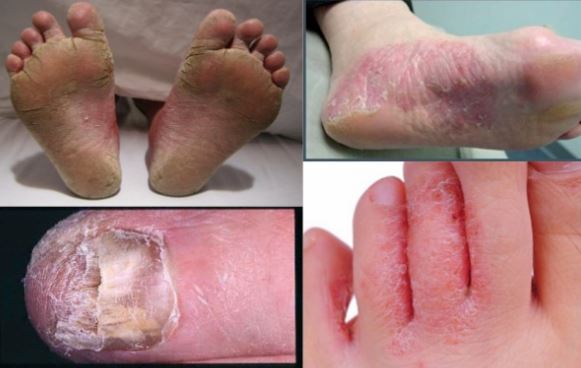
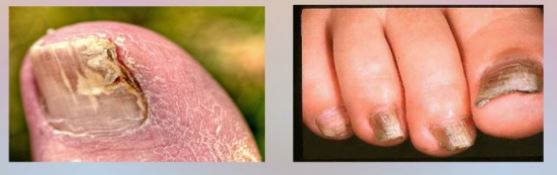
References
- Derrer, D. T. (2014, September 21). Fungal Infections of the Skin. Retrieved from WebMD: http://www.webmd.com/skin-problems-and-treatments/guide/fungal-infections-skin
- Kid’s Health. (2016). Athelete’s Foot. Retrieved from Kid’s Health: http://kidshealth.org/en/kids/athletes-foot.html
- Cole, G. (2016, April 29). Athlete’s Foot. Retrieved from Medicine Net: http://www.medicinenet.com/athletes_foot/page2.htm
- DermNet NZ. (2016, April 25). Tinea Pedis. Retrieved from DermNet NZ: http://www.dermnetnz.org/fungal/tinea-pedis.html
- ICD10 Data. (2015). Tinea pedis. Retrieved from ICD10 Data: http://www.icd10data.com/ICD10CM/Codes/A00-B99/B35-B49/B35-/B35.3
- The Healthline Editorial Team. (2015, October 19). Athlete’s Foot. Retrieved from Healthline: http://www.healthline.com/health/athletes-foot#Overview1
- Group, E. (2015, September 25). Home Remedies for Athletes Foot. Retrieved from Global Healing Center: http://www.globalhealingcenter.com/natural-health/athletes-foot-home-remedy/
