Torus Mandibularis
What is Torus Mandibularis?
Torus mandibularis or mandibular torus, tori mandibularis for plural, is a sublingual protuberance or a benign bony growth occurring on the mandible lingual side. Around 80% to 90% of these lesions present bilaterally near the bicuspid and tricuspid teeth and superior to the mylohyoid muscle, a paired muscle for mandibular attachment.
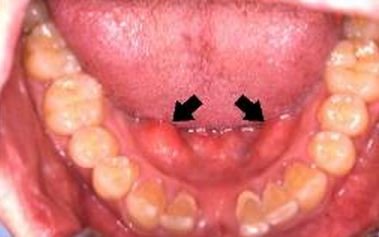
Image 1 – Torus Mandibularis (black arrows)
Cases of mandibular tori are usually asymptomatic though some patients usually complain of pain with denture placement and when food is lodged or forced against the lesions. These body growths are covered in the typical oral mucosal layers which are more often non tender without any drainage.
Mandibular tori gradually grow as nodular multilobulated mass occurring as single or multiple growths usually limited up to 2mm in size with largest documented diameter of 3 to 4cm. the growth size of these lesions vary but is some cases, the masses can grow large enough toward midline of the mouth.
On pathological examination, the torus has a dense bone presentation with a laminated pattern. The exotoses is composed of closed-pack, lamellar bone with a repeating compact concentric form. They are filled with scattered osteocytes, the cells of mature osseous or bone tissues, with tiny marrow spaces which are infused with fat marrow or loose fibrovascular tissue layers.
They may also come with thin margin of compact bone lying above inactive trabecular or spongy bone with red or yellow marrow. Limited osteoblastic activity is known in the lesions but most have active periosteal formation.
Majority of the body growth area exhibit expanded lacunae with condensed degenerating osteocytes which indicate bone ischemia. Ischemic damage is accompanied by fibrotic damage and enlarged veins in the marrow.
Tori can be mistaken as other kinds of bone proliferating soft tissue lesions. Hence, differential diagnosis covers presence of abscess, peripheral ossifying fibroma, vascular neoplasms, salivary gland malignancy, and bone cancer.
Torus Mandibularis Causes
The direct cause of torus mandibularis is still unknown although several factors are believed to contribute to its occurrence. It is usually genetically predisposed with autosomal dominant pattern which is more common among Inuits and Asians, particularly Koreans.
The lesions are predominant among males with an average onset between the fourth to the fifth decade of life. Torus palatinus, another variation of growth in the palatine process, is more usual to the female population. The prevalence rate of tori is around12.3% to 26.9% in adults and it rarely occurs among children with low prevalence of 3%.
Mandibular torus is developmental anomaly which becomes symptomatic in adulthood and continuously grows throughout life. It could be the result of mandibular arch torqueing and mandibular occlusal pressure. The pressure against the periodontal ligament due to factors like bruxism or teeth grinding and mastication pressure related to consumption of coarse food adding stress to the bicuspids could lead to abnormal bone formation at the lingual area.
Torus Mandibularis Treatment (removal/Surgery)
It is usually unnecessary to remove mandibular tori unless the lesions are large enough to interfere with oral functions such as dental placement, dental procedures, and mastication impairment. An isolated documented patient had difficult intubation due to large bilateral tori.
Recurrent traumatic oral mucosal ulceration on the area, which could be associated with mastication of sharp, hard food, is another indication for removal.
Torus mandibularis is managed my maxillofacial surgeons through mallet and chisel surgical removal. This procedure corresponds to burring or saw technique to reduce or eliminate the body growth and requires induction of general anesthesia. The treatment involves chiseling off the tori cortex or cutting through the base of the mass through a burring procedure.
Minimal postsurgical complications are expected with incidence of minimal bleeding, inflammation, and infection. Cases present with good prognosis and patient’s full recovery from the surgical incision is around 3 to 4 weeks.
Several cases report recurrence of lesions but this kind of growth has no potential for malignancy transformation. Recurrence is triggered by continuous pressure against the premolar or bicuspid teeth and surrounding mucosal area.
In cases of multiple bony lesions that are not typical of tori and other buccal lesions or exostosis, patients should be evaluated further for Gardner syndrome also known as familial adenomatous polyposis, an inherited disease which presents with colorectal polyps and extacolonic lesions.
References:
Durrani, M. and Barwise, J. (2000). Difficult endotracheal intubation associated with torus mandibularis. Anesthesia and Analgesia. 90 (3): 757-759. Retrieved from http://journals.lww.com/anesthesia-analgesia/pages/imagegallery.aspx?year=2000&issue=03000&article=00045
Garcia-Garcia, A, Martinez-Gonzalez, J., Gomez-Font, R. et al. (2010).Current status of the torus palatines and torus mandibularis.Medicina Oral, Patologia Oral, y Cirugia Oral. 15 (2): 353-360. Retrieved from http://www.ncbi.nlm.nih.gov/pubmed/19767716
Jainkiitivong, A. and Langlais, R.(2000). Buccal and palatal exostoses: prevalence and concurrence with tori. Oral Surgery, Oral Medicine, Oral Pathology, Oral Radiology and Endodontology. 90: 48-53. Retrieved from http://www.ncbi.nlm.nih.gov/pubmed/10884635
Mayhall, J., Dahlberg, A., and Owen, D. (1970).Torus mandibularis in an Alaskan Eskimo population. American Journal of Physical Anthropology, 33: 57-60. Retrieved from http://www.onlinelibrary.wiley.com/doi/10.1002/ajpa.1330330109/pdf
Neville, B.W., D. Damm, C. Allen, J. Bouquot.(2002). Oral & Maxillofacial Pathology.Second edition.Page 21. ISBN 0-7216-9003-3.
Ossenberg, N. (1981). Mandibular torus: a synthesis of new and previously reported data and discussion of its cause. Contributions to Physical Anthropology, Ottawa.1-52.
Pynn, B., Kurys-Kos, N., Walker, D., and Mayhall, J. (1995). Tori mandibularis: a case report and review of the literature. JCDA: Journal of the Canadian Dental Association, Canada. 61:1057-1058, 1063-1066.
Sauret, J. and Ahiarah, A. (2011).Torus Mandibularis.Consultant 360. Retrieved from http://www.consultant360.com/content/torus-mandibularis
Unterman, S. and Fitzpatrick, M. (2010).Torus mandibularis.Western Journal of Emergency Medicine, Chicago. 11 (5): 520. Retrieved from http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3027453/
